Are You Making These 7 Common CPR Certification Mistakes?

Getting your CPR certification is one of the most proactive steps you can take to protect your family, coworkers, and community. However, simply showing up to a class doesn’t guarantee you’ll walk away with the skills—or the confidence—to save a life. Many students fall into the same traps, leading to ineffective techniques or even failing their practical exams.
At CPR Classes Near Me, we’ve seen thousands of students walk through our doors. We’ve noticed a pattern in where people struggle most. Whether you are a first-timer or a seasoned pro looking for a renewal, understanding these common pitfalls is the first step toward mastery.
In this guide, we’ll dive deep into the most frequent CPR certification mistakes and, more importantly, how you can avoid them to ensure you’re ready when the clock is ticking.
Why is proper hand placement so important?
One of the most frequent errors we see in the classroom is incorrect hand placement. It sounds simple—place your hands in the center of the chest—but in the heat of a timed assessment, many students drift.
Some students place their hands too high, near the neck, or too low, over the stomach (xiphoid process). Placing hands too low can cause internal injuries, such as a fractured breastbone or damage to the liver, rather than effectively pumping the heart.
To avoid this:
- Locate the “Nipple Line”: For an adult, the center of the chest between the nipples is your target.
- Use the Heel of Your Hand: Only the heel of your bottom hand should touch the chest. Interlace your fingers and pull them upward so they don’t press against the ribs.
- Lock Your Elbows: Keep your arms straight and your shoulders directly over your hands. This allows you to use your body weight rather than just your arm strength.
Are your compressions deep enough to save a life?
“Push harder” is the most common phrase heard in a CPR class. It is human nature to be afraid of hurting the person you are trying to help. Students often perform “shallow” compressions because they are worried about breaking ribs.
However, if you don’t compress the chest at least 2 inches for an adult, the blood simply won’t reach the brain. During certification, manikins are designed with internal “clickers” or lights to tell you if you’ve hit the right depth. If you don’t hear that click, you aren’t doing effective CPR.
How to get it right:
- Trust the Manikin: Use the practice time to find the “sweet spot” where the click occurs.
- Accept the Risk: Understand that ribs may crack during real CPR, and that is a secondary concern compared to a stopped heart.
- Lean Into It: Use your upper body weight to drive the compression. If you find yourself getting tired quickly, you’re likely using only your arms.
Is your compression rate too fast or too slow?
Timing is everything. If you go too slow, you won’t maintain enough blood pressure to keep the brain alive. If you go too fast (over 120 beats per minute), the heart doesn’t have enough time to refill with blood between squeezes.
Many students get nervous and start pumping as fast as they can, which is a recipe for exhaustion and ineffective resuscitation.
To stay on track:
- Think of the Music: The classic song “Stayin’ Alive” by the Bee Gees is 103 beats per minute—the perfect pace. Other options include “Dancing Queen” by ABBA or “Just Dance” by Lady Gaga.
- Count Out Loud: “One, two, three, four…” Counting out loud helps you maintain a steady rhythm and keeps your breathing regulated.
- Practice with a Metronome: Many modern CPR classes use metronomes or apps to help students internalize the 100–120 BPM rhythm.
Do you forget to let the chest recoil?
This is the “silent killer” of effective CPR. Recoil is the act of letting the chest come all the way back up to its neutral position after a compression.
Many students “lean” on the chest. This means they never fully release the pressure between compressions. If the chest doesn’t fully recoil, the heart can’t refill with blood. It’s like trying to pump a half-empty bellows—you’re working hard, but very little is happening.
How to avoid leaning:
- Lighten the Load: After the downward push, make sure your weight is completely off the manikin, though your hands should remain in contact with the skin so you don’t lose your placement.
- Think “Up and Down”: Focus as much on the “up” motion as you do on the “down” motion.
- Check Your Posture: If you are leaning too far forward, you’ll naturally keep weight on the chest. Ensure your shoulders are directly over your hands, not in front of them.
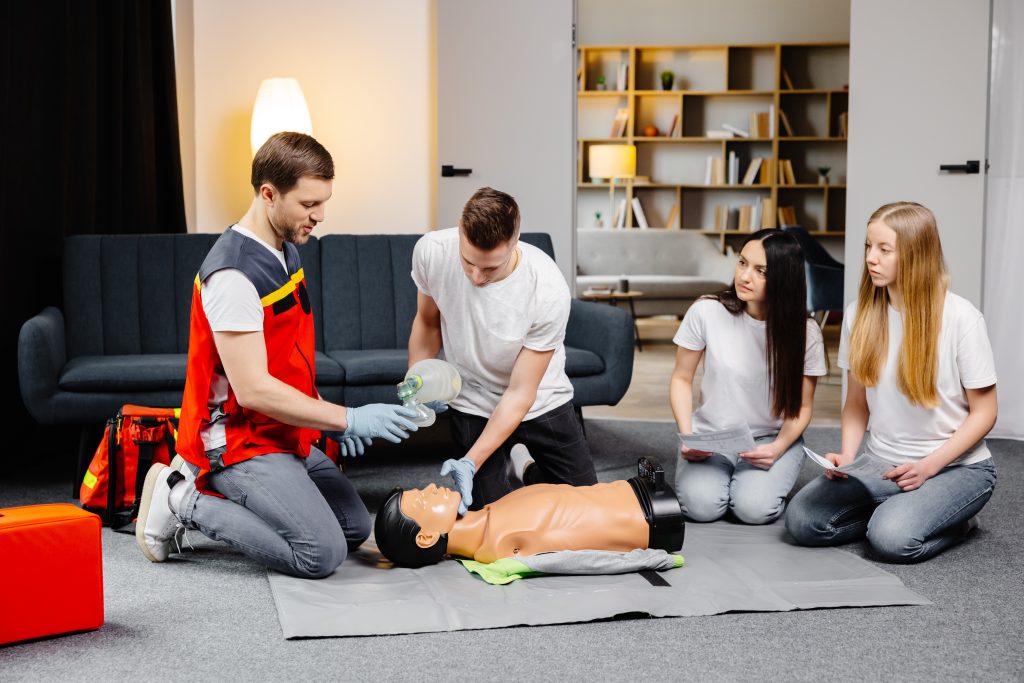
Are you over-inflating the lungs during rescue breaths?
While many layperson classes focus on “Hands-Only CPR,” most certification levels still require rescue breaths. A common mistake is blowing too much air or blowing too hard into the victim.
Over-inflating the lungs can cause air to enter the stomach (gastric inflation). This often leads to vomiting, which can block the airway and create a much messier, more dangerous situation.
To give perfect breaths:
- Watch the Chest: You only need to provide enough air to see the chest visibly rise. As soon as it starts to lift, stop blowing.
- One Second Each: Each breath should last about one second.
- Tilt the Head: Ensure you are using the “head-tilt, chin-lift” maneuver to open the airway properly. If the airway isn’t open, the air won’t go in no matter how hard you blow.
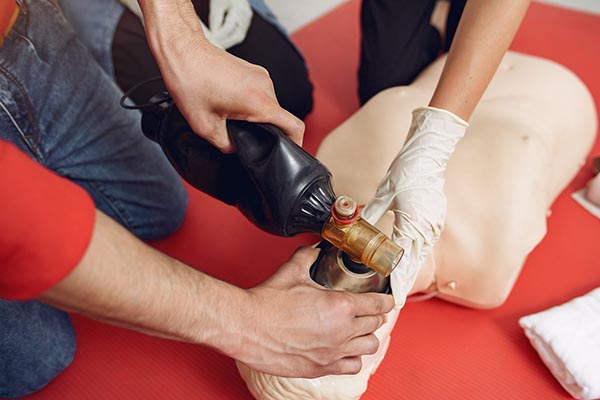
Why do students hesitate to use an AED?
In a certification class, the Automated External Defibrillator (AED) is often the part that makes students the most nervous. They worry about “zapping” someone who doesn’t need it or getting the pads in the wrong place.
The truth is, an AED is designed to be foolproof. The biggest mistake is delaying its use. Every minute that passes without a shock (if one is needed) decreases the chance of survival by about 10%.
To master the AED:
- Turn it on immediately: As soon as the device arrives, power it up. It will talk you through the rest of the steps.
- Follow the pictures: The pads have clear diagrams showing exactly where to place them.
- Clear the area: Ensure no one is touching the person when the AED is analyzing the rhythm or delivering a shock.
Is your certification actually valid?
Believe it or not, one of the biggest “mistakes” happens before you even step into a classroom: choosing the wrong course. There are many “online-only” certifications that claim to be valid but are not accepted by employers or OSHA because they lack a hands-on skills assessment.
If you need a certification for work—whether you are a teacher, a construction worker, or a coach—you must ensure the course includes an in-person component with a certified instructor.
How to choose correctly:
- Check Accreditation: Look for courses backed by the American Heart Association (AHA) or the American Red Cross.
- Avoid “Instant” Online Certificates: If there is no manikin involved, your employer likely won’t accept it.
- Verify the Type: Ensure you are taking a “Provider” level course if required for your job, rather than just a general awareness class.
How can you summarize these common errors?
To ensure you are fully prepared, it is helpful to look at these mistakes as a checklist for your next practice session. Avoiding these specific errors will significantly improve your chances of passing your exam and saving a life.
- Hand Placement: Instead of drifting toward the ribs or neck, keep your hands centered between the nipples to avoid internal injury.
- Compression Depth: Don’t be afraid to push. You must reach at least 2 inches to circulate blood; use the manikin’s feedback lights or clicks as your guide.
- Rhythm and Pace: Avoid the urge to rush. Stay between 100 and 120 beats per minute by using a song or metronome to guide your speed.
- The Recoil Phase: Remember that the heart fills when you let go. Never lean on the chest; allow it to return to its natural height after every push.
- Ventilation Volume: Don’t over-inflate. Stop your rescue breath the moment you see the chest rise to prevent stomach inflation and vomiting.
- AED Speed: Never wait to use an AED. The moment it is available, turn it on and let the voice prompts lead the way.
- Course Choice: Avoid the “online only” trap. Ensure your certification includes an in-person skills check to meet workplace requirements.
Conclusion
Mastering CPR isn’t about being a medical genius; it’s about muscle memory, composure, and following the most up-to-date guidelines. By being aware of these common certification mistakes—like leaning on the chest or pushing too shallowly—you can focus your training on the techniques that actually save lives.
When you train with CPR Classes Near Me, our experienced instructors are dedicated to catching these mistakes early. We provide the hands-on feedback you need to feel confident, not just during your test, but in a real-world emergency. Don’t wait until a crisis happens to realize your technique is off.
Ready to get certified the right way? Contact CPR Classes Near Me today to find a local, accredited class that fits your schedule!
Frequently Asked Questions (FAQ)
Can I fail a CPR certification class?
Yes, it is possible to fail if you cannot demonstrate the physical skills required by the certifying body. This usually involves failing to reach the correct compression depth, rate, or failing to use the AED safely. However, a good instructor will work with you during the practice session to ensure you are ready before the final test.
Do I have to do mouth-to-mouth during the test?
In most certified “Healthcare Provider” or “Professional Rescuer” courses, rescue breaths are required. However, many “Heartsaver” or layperson courses focus on “Hands-Only” CPR. Most classes will provide a pocket mask or a barrier device so you are never in direct contact with the manikin’s mouth.
What happens if I break a rib during CPR?
In a real-life emergency, breaking a rib is a common side effect of high-quality CPR. The priority is to circulate blood to the brain. Most “Good Samaritan” laws protect rescuers from liability for such injuries during life-saving attempts. In a certification class, you practice on manikins to learn the right amount of force to use.
How often do I need to renew my certification?
Most CPR certifications are valid for two years. Because guidelines are updated periodically and physical skills can degrade over time, you must take a renewal course every 24 months to remain “current.”
Are online-only CPR certifications legitimate?
While online courses provide great theoretical knowledge, most employers and regulatory bodies (like OSHA) do not recognize “online-only” certifications. To be fully certified, you almost always need a “Blended Learning” approach where you complete the theory online but perform the physical skills in front of a certified instructor.